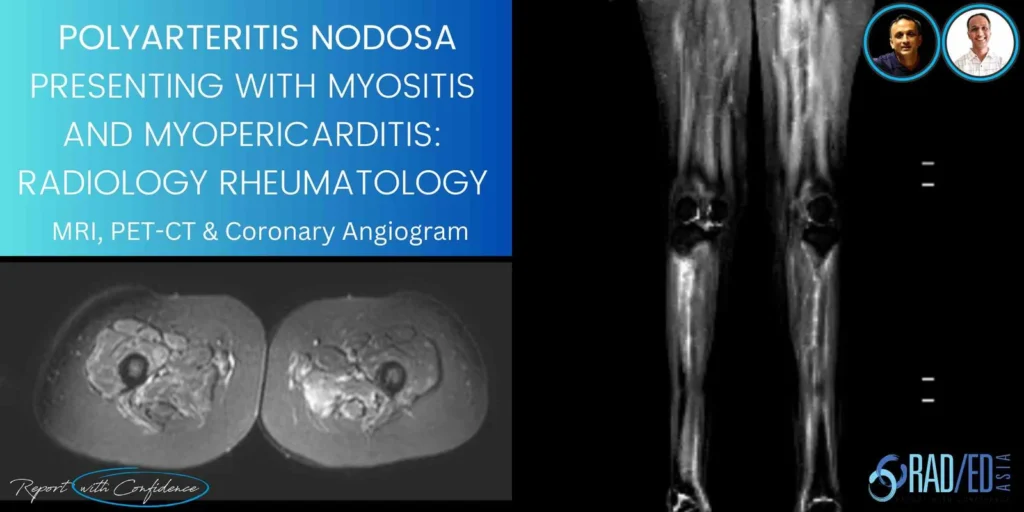
POLYARTERITIS NODOSA WITH MYOPERICARDITIS AND MYOSITIS : MRI PET CT & CORNARY ANGIOGRAM FINDINGS

A combined Clinico Radiological case from Dr Joe Thomas (Rheumatologist)
This is a combined case with Dr Joe Thomas on a case of Polyarteritis Nodosa that presented with Myositis and Myopericarditis. Dr Thomas is a senior consultant Rheumatologist who is also joining us in presenting the Spine Arthropathy and Spondyloarthropathy course.
- 20-year-old student presented with polyarthritis.
- ESR 38, CRP 11, ANA(IF) speckled 2 +, ANA profile showed ds DNA 2 + and SCL 70 1+, dsDNA positive by elisa (461).
- Diagnosed as SLE and was on treatment with HCQS, steroids, methotrexate.
- Persistent joint pain with fever and rising inflammatory markers (ESR 90, CRP121) despite treatment.
- PET CT : Inflammatory arthritis with enthesitis.
- Managed with pulse steroid and rituximab 500mg.

- Readmitted in view of persistent fever and generalized myalgia in functional class 4.
- Inflammatory markers- ESR 120, CRP 201.
- Work up for infection and malignancy were negative (including bone marrow).
- Steroids and IVIG were started.
- Developed left lower limb numbness with gait abnormality and severe retrosternal chest pain.

- Admitted in ICU in view of severe chest pain (requiring opioids to control pain).
- Very high inflammatory markers, Trop I- 740.0 ng/L (N<9) and repeat work up for Lupus was negative.
- ECHOCARDIOGRAM: Global LV hypokinesia with severe left ventricular systolic dysfunction.
- Diagnosis at this stage was severe myopericarditis secondary to autoimmune disease.

- USG guided Muscle biopsy done suggestive of inflammatory myositis.
- Surprisingly CPK and other work up for myositis was negative.
- There was worsening mononeuritis multiplex.
- In spite of repeat pulse steroids, her chest pain, cardiac function and cardiac enzymes worsened.

Polyarteritis Nodosa With Myopericarditis.

- In this case clinical phenotype was that of PAN rather than lupus inspite of initial autoantibody profile, (main clue was >CRP 100).
- In a patient with myalgia/no muscle weakness and MRI suggestive of myositis, with normal CPK, think of PAN.
- Work up for DADA2 and another genetic syndrome were negative. The patient stabilized with combination of medications (Steroids + IVIG + Tofacitnib + Methotrexate).

For all our other current MSK MRI & Spine MRI
Online Guided Mini Fellowships.
Click on the image below for more information.
- Join our WhatsApp RadEdAsia community for regular educational posts at this link: https://bit.ly/radedasiacommunity
- Get our weekly email with all our educational posts: https://bit.ly/whathappendthisweek















